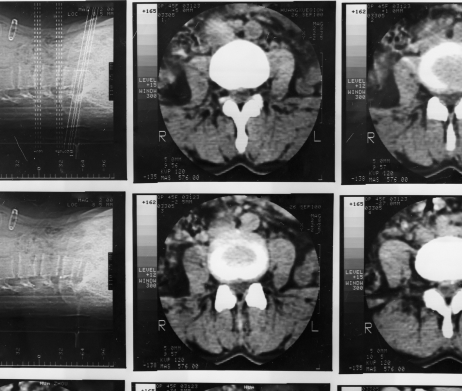
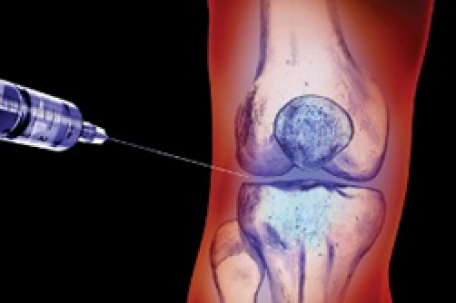
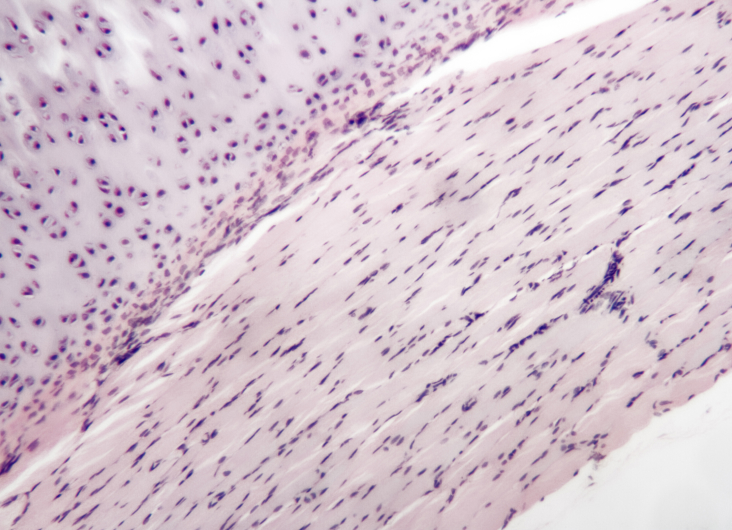
Osteoarthritis is the most common form of arthritis and affects millions of people worldwide, causing debilitating conditions for patients suffering from this degenerative condition. Although the risk of developing osteoarthritis increases with age, many young people also suffer from it due to sports injuries, lifestyle and other factors. The joints that can be affected are major joints in the limbs, such as elbow and fingers, toes, ankle, knee and hip as well as regions of the cervical spinal cord. Chondrocyte damage is non-reversible, and if left untreated it leads to permanent defects of the bones and joints.